Missing teeth affect more than appearance — they change how you eat, speak, and even how your face supports itself. Whether tooth loss is the result of decay, gum disease, or injury, modern implant dentistry offers a way to rebuild a smile that looks natural and performs reliably. Our approach emphasizes predictable outcomes and long-term oral health so patients can regain comfort and confidence.
The process begins with a careful evaluation of your oral and overall health. We consider bone volume, gum condition, and bite dynamics to design a treatment that meets your functional and aesthetic goals. When planned well, implants replace missing tooth roots and support restorations that behave like real teeth.
For many people, implants are not just a cosmetic fix — they are a practical solution that preserves facial structure and chewing ability. The team at Draper Dental combines current surgical techniques with high-quality restorative materials to deliver results that integrate seamlessly with your natural teeth.

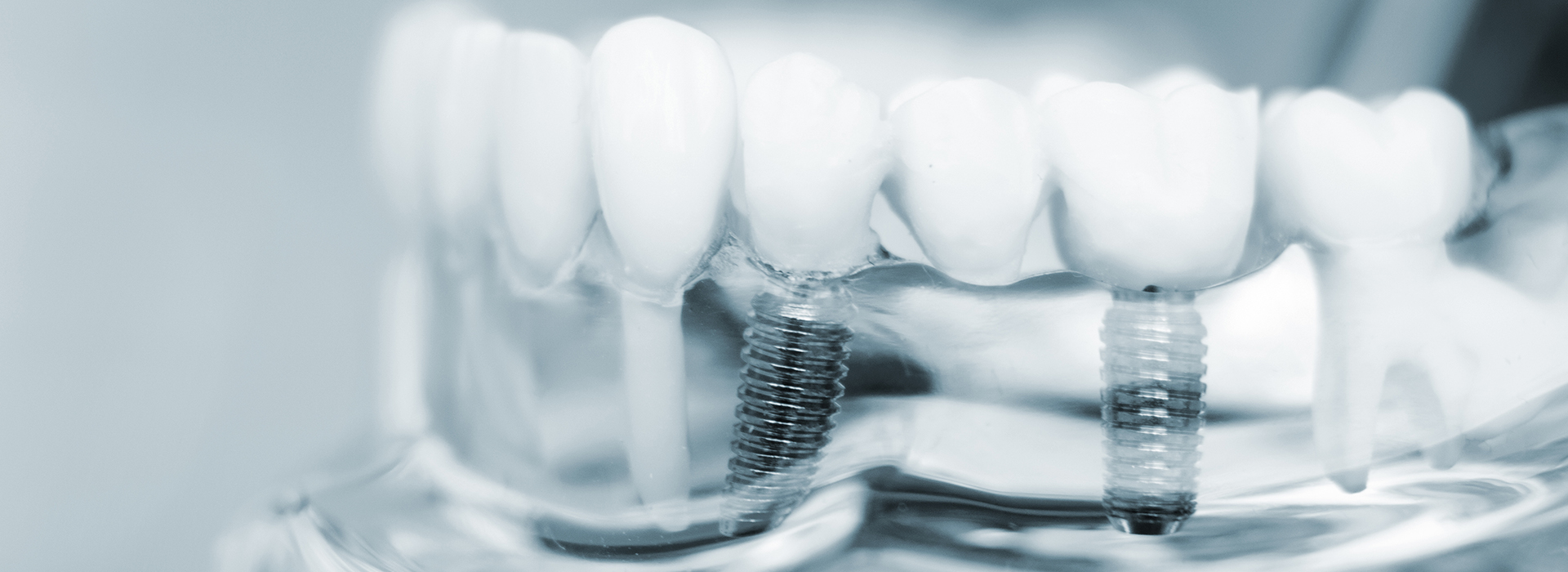
Dental implants are anchored into the jawbone using biocompatible titanium posts that act like tooth roots. Over time the bone bonds to the implant surface in a process called osseointegration, creating a stable foundation for crowns, bridges, or full-arch prostheses. This integration is what gives implants their strength and durability.
Because implants transfer chewing forces to the jawbone similarly to natural roots, they help preserve bone density and facial contours. That structural benefit reduces the sunken appearance that can accompany long-term tooth loss and helps maintain a balanced bite and jaw function.
The visible portion of an implant restoration — a crown, bridge, or denture — is crafted to match your remaining teeth in color, shape, and size. With precise planning and custom prosthetic work, implants become indistinguishable from natural teeth both in appearance and in daily use.
At their core, dental implants are made of three parts: the implant (the post placed in bone), an abutment (a connector), and the prosthetic tooth or teeth (crown, bridge, or denture). Each component plays a role in replicating the function of a natural tooth and restoring the smile.
Advances in imaging and digital planning allow for highly accurate placement that minimizes surgical time and improves restorative outcomes. With clear communication and careful scheduling, many patients move through the stages of care with predictable healing and excellent function.
Implants offer a range of benefits beyond replacing a missing tooth. They provide a fixed, stable solution that reduces the need for removable appliances and preserves adjacent teeth that might otherwise have to be altered to support a bridge. For many patients, implants restore a sense of normalcy when eating, speaking, and smiling.
Because implants stimulate the bone, they help prevent the progressive bone loss that follows tooth extraction. That preservation supports facial structure over time and may reduce the need for more extensive reconstructive work later. Implants are also durable when maintained with proper hygiene and periodic professional care.
From a practical perspective, implants behave like the teeth they replace — they don’t slip, they don’t trap food in the same way removable devices can, and they allow patients to enjoy a varied diet without special precautions. These everyday improvements often translate into better overall quality of life.
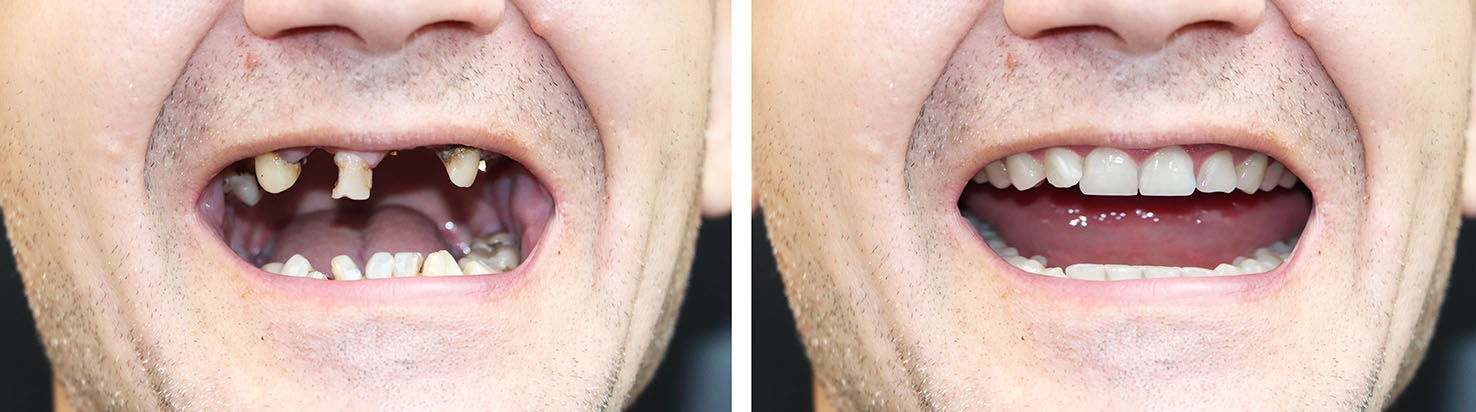
A single-tooth implant with a custom crown is often the most conservative option when one tooth is missing. Instead of preparing adjacent teeth for a bridge, an implant stands on its own and restores normal chewing forces while maintaining the health of neighboring teeth.
The crown is shaded and shaped to blend with your existing smile and the implant-supported tooth provides the same visibility, form, and function as the original tooth. This approach simplifies long-term care and protects natural tooth structure.
When more than one tooth is missing in a row, implant-supported bridges can replace several teeth without relying on adjacent natural teeth for support. Strategically placed implants act as anchors for a bridge of connected crowns, delivering strong, stable restoration while preserving bone beneath the replaced teeth.
This strategy maintains oral health and reduces the need to modify healthy teeth, which is often necessary with traditional bridges. It’s a restorative option that balances durability and conservation of natural structures.
For patients missing most or all teeth in an arch, a full-arch restoration supported by four or six implants provides a non-removable replacement that feels like natural teeth. These fixed prostheses restore chewing function and facial support without the daily removal required by conventional dentures.
In many cases, temporary prostheses can be attached immediately after implant placement to restore appearance and function while the implants integrate. Final prosthetics are then fitted once healing is complete to ensure precise occlusion and aesthetics.
Implant-retained dentures use several implants as stable attachment points for an overdenture. This hybrid approach significantly improves retention and comfort compared with traditional removable dentures while still allowing the appliance to be removed for cleaning.
For many patients who prefer the ease of a removable prosthesis, implant retention offers a meaningful upgrade in stability and confidence when speaking and eating.
Successful implant care begins with a thorough clinical and radiographic assessment. Digital imaging, bite records, and an evaluation of your health history enable us to create a detailed plan that maps implant locations, restorative needs, and any preparatory procedures that may be required.
Clear planning also allows the team to discuss timelines and to coordinate any grafting or extractions so each step supports the next. Communication is central: informed patients know what to expect at every appointment and can participate in treatment decisions.
Implant placement is typically performed in an outpatient setting with local anesthesia and, when appropriate, conscious sedation options to maximize comfort. The surgical procedure involves placing the implant into the prepared site and securing it for healing. After the procedure, most patients experience manageable discomfort that improves over several days.
We provide clear post-operative instructions, and follow-up visits ensure that healing is progressing as planned. In many cases, a temporary restoration can be provided so you leave the appointment with a natural-looking smile.
After osseointegration — the period during which bone bonds to the implant — the final restoration is fabricated and attached. This stage focuses on precise fit, occlusion, and esthetics so your bite feels natural and your smile looks harmonious.
Long-term maintenance involves regular dental visits, good oral hygiene, and occasional professional cleanings tailored to implant care. With appropriate follow-up, implants can serve as a stable, long-term foundation for oral health.
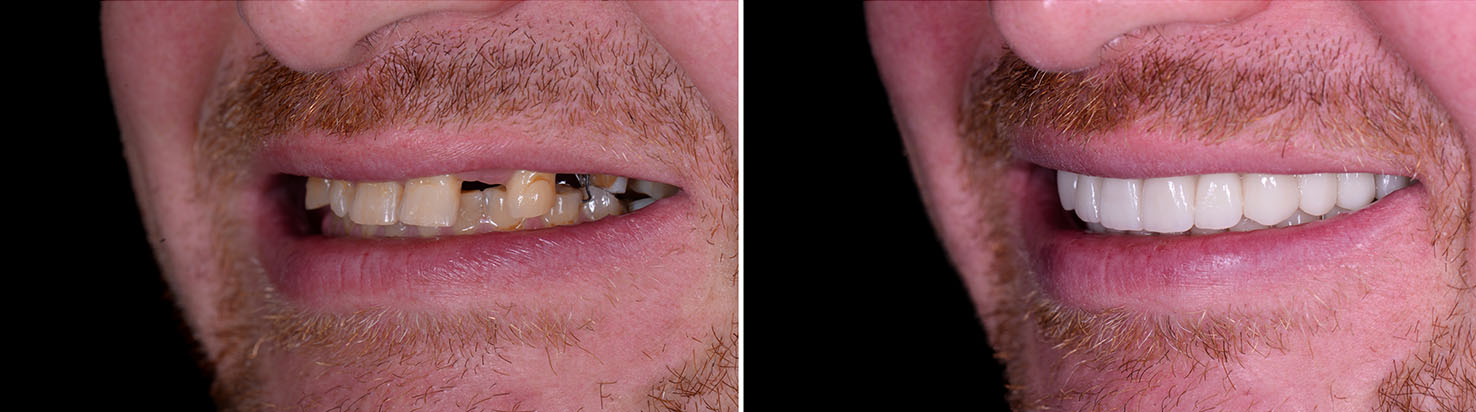
Healthy, adequate bone is essential for implant stability. When bone volume has diminished after tooth loss or disease, bone grafting can rebuild the site to provide the support implants require. Grafts use safe, proven materials to promote new bone growth and create a reliable foundation for later implant placement.
The decision to graft depends on the size and quality of the available bone and the long-term goals for the restoration. When grafting is recommended, it is planned carefully and timed to optimize healing and implant integration.
Overall health affects healing. Conditions such as uncontrolled diabetes, heavy tobacco use, or certain medications can influence treatment decisions and timelines. During the evaluation, we review medical history and, when needed, collaborate with medical providers to ensure a safe and effective plan.
Even when complicating factors exist, many patients can still pursue implant solutions with tailored protocols that address specific risks and support successful healing.
Once implants are restored, ongoing care helps preserve both the implant and surrounding tissues. Daily brushing, interdental cleaning, and routine dental visits for professional assessment and hygiene are vital. Our preventive protocols focus on detecting early signs of complications and maintaining healthy soft tissue around the implants.
With consistent home care and periodic professional attention, implants provide a dependable foundation for a functional, attractive smile for many years.
Replacing missing teeth is a significant step toward restoring oral health, comfort, and self-assurance. Implant dentistry provides versatile solutions tailored to individual needs, from single-tooth restorations to full-arch rehabilitations. We combine thoughtful planning, modern techniques, and attention to detail to deliver outcomes that align with each patient’s expectations.
If you would like to learn more about how implant dentistry could help you, please contact us for additional information or to schedule a consultation. Our team is here to answer your questions and help you determine the best path forward for your smile.
If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Dental implants are engineered tooth replacements that consist of a biocompatible implant post, an abutment and a custom prosthetic such as a crown, bridge or denture. The implant post is placed into the jawbone to act as a new root and provide a stable foundation for the restoration. By restoring root function, implants help reestablish chewing efficiency and support surrounding soft tissues.
After placement the bone bonds to the implant surface through osseointegration, creating long-term stability for the restoration. The visible prosthetic is crafted to match adjacent teeth in color, shape and size so it blends naturally with your smile. Because implants transmit biting forces to the bone like natural roots, they also help preserve bone volume and facial contours over time.
A good candidate typically has healthy gums, adequate jawbone volume and overall medical stability to support healing after surgery. Patients with controlled chronic conditions can often proceed with implants when their medical care is coordinated and risks are managed. The clinical evaluation includes a review of medical history, medications and lifestyle factors that influence healing and treatment planning.
Certain issues such as uncontrolled diabetes, heavy tobacco use or medications that affect bone healing may require additional planning rather than disqualifying a person outright. In many cases, preparatory procedures like bone grafting or soft-tissue augmentation can create the conditions needed for successful implant placement. The recommendation balances functional goals, anatomical realities and long-term tissue health.
Implant options include single-tooth implants with custom crowns, implant-supported bridges for multiple adjacent teeth and full-arch fixed restorations that replace most or all teeth in an arch. Implant-retained overdentures offer a hybrid solution that improves denture stability while remaining removable for cleaning. Treatment selection depends on bone quantity, patient preferences and the desired balance between fixed and removable solutions.
Modern digital planning and prosthetic materials allow clinicians to tailor restorations for esthetics and function, and in some cases provide immediate provisional teeth. Decisions about the number and placement of implants, prosthesis type and staging are guided by both surgical and restorative considerations. Your dentist will explain the advantages and limitations of each approach to identify the best option for your situation.
The overall timeline varies based on case complexity, the need for preparatory work and the chosen restoration. Simple cases without grafting may move from placement to final restoration within a few months, while cases requiring bone grafting or staged reconstruction may take longer to allow for predictable healing. Immediate provisional restorations are possible for select patients, but timelines are individualized to protect long-term outcomes.
Osseointegration — the period when bone fuses to the implant — is a major factor in scheduling the final prosthetic and often determines the interval between surgery and restoration. Regular follow-up visits enable clinicians to confirm integration and proceed when conditions are optimal. Clear communication about milestones helps patients plan around appointments and temporary limitations during recovery.
Adequate bone volume and healthy soft tissue are essential for predictable implant placement, and when deficiencies exist bone grafting or soft-tissue augmentation can rebuild the site. These procedures use proven materials and techniques to promote new bone and tissue growth and create a stable foundation for implants. The decision to graft depends on the size and quality of available bone, the location of the missing tooth and the long-term goals for the restoration.
Grafting may be performed before implant placement or at the time of surgery depending on the clinical situation and treatment plan. Common techniques include ridge augmentation, sinus lifts and connective tissue grafts that address specific anatomical needs. Digital imaging and careful planning help determine whether grafting is recommended and how it affects the treatment timeline.
Implant placement is typically performed in an outpatient setting using local anesthesia and optional conscious sedation to maximize comfort. The surgical procedure involves placing the implant into a prepared site, and most patients experience manageable discomfort that improves over several days with rest and conservative self-care. Postoperative instructions and timely follow-up visits are provided to monitor healing and address any concerns.
Swelling and mild soreness are common in the first 48 to 72 hours and are usually controlled with ice, rest and recommended medications. Temporary restorations are often provided when appropriate so patients do not leave treatment visibly missing teeth. If prolonged pain, fever or unusual bleeding occurs, prompt contact with the dental team ensures timely evaluation and care.
Long-term implant success depends on consistent home care and routine professional maintenance focused on both the restoration and surrounding tissues. Daily brushing, interdental cleaning with floss or specialized brushes and gentle cleaning beneath implant-supported prostheses help control plaque and reduce the risk of peri-implant disease. Avoiding tobacco and managing systemic health issues further supports tissue stability around implants.
Regular dental visits allow clinicians to monitor soft tissue health, check occlusion and provide professional hygiene tailored to implants. Periodic radiographs may be used to evaluate bone levels and detect early changes that warrant intervention. With good self-care and scheduled follow-up, implants commonly provide many years of reliable function.
Implant therapy is well established but carries potential risks including infection, delayed healing or failure of integration in some cases. Rare complications such as nerve injury or sinus involvement can occur if anatomy is not carefully evaluated and respected. Thorough preoperative assessment and digital planning reduce these risks and support safer surgical outcomes.
Peri-implantitis is an inflammatory condition that can affect the tissues around an implant if plaque accumulates and is not addressed. Preventive measures like excellent oral hygiene, routine professional care and early attention to soft tissue changes significantly lower the likelihood of complications. When problems are detected early, a range of treatments can often stabilize the site and preserve the implant.
When placed and maintained properly, dental implants can last for many years and are considered a long-term tooth replacement option. Longevity depends on factors such as oral hygiene, tobacco use, systemic health, the quality of the restoration and the precision of surgical and prosthetic work. Regular maintenance and monitoring play a central role in preserving implant health and function.
The experience of the treatment team and adherence to evidence-based protocols also influence outcomes, and the team at Draper Dental emphasizes personalized maintenance plans to support implant longevity. Early detection of tissue changes and prompt intervention help address problems before they compromise the restoration. Patients who combine diligent home care with professional follow-up typically experience the best long-term results.
A consultation begins with a comprehensive review of your dental and medical history, an oral exam and digital imaging to evaluate bone volume, gum health and bite relationships. The clinician discusses your goals, explains relevant treatment options and outlines any preparatory steps that may be necessary for a successful outcome. This visit also provides an opportunity to review anesthesia options, expected timelines and postoperative care so you can make an informed decision.
At Draper Dental the consultation is designed to produce a personalized plan that aligns functional needs with esthetic goals while prioritizing tissue health. Digital planning tools and clear communication help patients understand the proposed sequence of care and what to expect at each stage. If you decide to proceed, the team will coordinate appointments and preparations to support predictable healing and restoration.
Phone:
Email: